Prostate cancer
Prostate cancer is the commonest cancer in the UK and the second most common cause of male cancer deaths. Each year nearly 50,000 men are diagnosed and over 11,000 die from the disease. Despite these figures, for most men prostate cancer grows slowly and is commonly confined to the prostate, resulting in high cure rates.
At present there are 3 established risk factors for prostate cancer:
- Age. Risk increases with age from 40 years upwards.
- Family history. Men with one first-degree relative (father, brother) have double the average risk. If 2 or more first-degree relatives are diagnosed the risk may be up to seven times higher.
- Ethnicity. Afro-Caribbean and black African are at increased risk, whereas Asian men generally have a lower risk.
Symptoms and signs of prostate cancer
It is important to point out that there are usually no signs or symptoms in the early stages of prostate cancer.
However, prostate cancer may occasionally present with following signs (which are also symptoms of non-cancer prostate disease such as benign prostatic hyperplasia (BPH).
- The need to pass urine more frequently, often during the night.
- The need to rush to the toilet.
- Difficulty in starting to pass urine (hesitancy).
- Straining or taking a long time while passing urine.
- A weak flow of urine.
- Feeling that your bladder has not emptied fully.
Sometimes men only realise something is wrong once the cancer starts to spread. These symptoms may include:
- Blood in the urine (haematuria).
- Bone and back pain.
- Pain when pass urine or ejaculating.
- Pain in the testicles.
- Weight loss
Diagnostic tests
A number of tests can be performed to assess the chances of a man having prostate cancer. The most commonly used are:
- Digital rectal examination. A digital rectal examination (DRE) is a short physical examination (<30 seconds) whereby a doctor inserts a gloved finger into the rectum to feel for lumps in the prostate.
- PSA. PSA stands for prostate specific antigen, which is a protein produced by the prostate which helps liquefy sperm. All men have a certain level of PSA, which can be measured by a simple blood test. A high PSA is commonly caused by infection, prostate enlargement, and prostate cancer.
- MRI. An MRI or magnetic resonance imaging scan is a non-invasive way of imaging the prostate to look for cancer. The scan takes approximately 45 minutes and commonly include and injection of contrast material that enhances the images.
- PSA Density. Calculated using PSA and volume of the prostate at MRI. A value less than 0.12 is associated with a lower risk of prostate cancer.
The only way to be certain of a prostate cancer diagnosis is by performing a prostate biopsy. There are a number of ways of doing this:
- Transrectal prostate biopsy. A traditional approach where needles are passed through the rectal wall to sample the prostate. Occasionally performed.
- Transperineal prostate biopsy. A newer approach where needles are passed through the skin between the anus and the scrotum. May be performed under local or general anaesthetic. Lower chance of infection when compared with transrectal biopsy.
Prostate cancer treatment
There are three main stages of prostate cancer:
- Localised - prostate cancer is confined to the gland
- Locally advanced - prostate cancer has grown outside of the prostate but has not spread to distant areas
- Advanced or metastatic - cancer has spread to distant areas, including lymph nodes and bones, and rarely liver, lung and brain.
Treatment options depend on the stage of the disease. For patients with localised disease and locally advanced disease there are a number of available treatment options to choose from, which can be very confusing. However, not all of these options will be suitable for an individual patient, and depend on a number of other factors including patient age, general health and personal preferences. Furthermore, some of the newer treatments are experimental and do not have long-term data.
Available options include:
- Active monitoring
- Radical prostatectomy
- Radical radiotherapy (external beam or brachytherapy)
- Experimental techniques (cryotherapy, high intensity focused ultrasound (HIFU))
- Hormone therapy alone
Active surveillance
Not all patients with prostate cancer required immediate treatment. This is because in many cases prostate cancer is slow growing and may not cause any problems during a patient's lifetime. Slow growing prostate cancers are typically low grade and low volume. Active surveillance is used to ensure that patients with these types of cancer are not treated unnecessarily. It involves monitoring the PSA blood test closely and repeating the MRI scan and prostate examinations at regular intervals. It is important to point out that active surveillance is not the same as ‘doing nothing’. If there are signs of progression your specialist will discuss the need for further additional treatments designed to cure the disease.
Radical prostatectomy
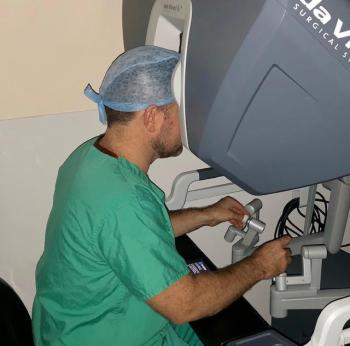
A radical prostatectomy is an operation performed by surgeons to remove the prostate and seminal vesicles in men with a diagnosis of prostate cancer. In most men the aim of radical prostatectomy is to remove all of the cancer, thereby providing a cure. Whilst prostatectomy may be performed safely by open or standard keyhole techniques, Nottingham Urology Group surgeons offer robotic-assisted radical prostatectomy using the da Vinci™ Surgical System.
The £2.2million da Vinci™ Surgical System, funded by Nottingham University Hospitals NHS Trust and the Nottingham Hospitals Charity was the first surgical robot to be introduced in the East Midlands. The system utilises high-definition 3D vision and articulated instruments to afford the surgeon an unprecedented level of precision and dexterity than ever before. In recent years, robotic prostatectomy has been shown to be safe and effective for prostate removal and it is now considered the gold standard for men requiring surgery for prostate cancer, associated with fewer complications, better outcomes and faster recovery times than traditional surgical techniques. Mr Tom Walton and Mr Ben Sherwood, both highly experienced Nottingham Urology Group specialist surgeons, offer da Vinci™ robotic prostatectomy, and can advise on whether surgery is right for you.
For more information about robotic-assisted radical prostatectomy please click here for our comprehensive RARP information sheet (650kb). Alternatively, if you wish to arrange an appointment to see one of our surgeons, please contact Spire Nottingham on 0115 9377801, or BMI Park Hospital on 0115 9662113.
Radical radiotherapy
Radical radiotherapy is suitable for men with localised and locally advanced prostate cancer. There are two main types: conventional external beam and brachytherapy. Radiotherapy is designed to preferentially kill prostate cancer cells whilst allowing normal prostate tissue to recover. In doing so, radiotherapy causes changes to the prostate, which means that surgery is usually not possible should the disease recur in the future.
External beam radiotherapy (EBRT)
The prostate is treated with high doses radiotherapy beams, which are aimed from outside the body at the prostate gland and the immediate surrounding tissues. This is done whilst a patient lies in the radiotherapy machine. The treatment takes place every day for a period of 4-7 weeks. EBRT is usually accompanied by treatment that blocks the effects of the male hormone testosterone.
EBRT is generally thought to be less suitable for younger, fitter men who have organ confined disease, although cure rates for EBRT have been shown to be equivalent which compared with surgery.
Brachytherapy
The prostate cancer is implanted with radioactive ‘seeds’ under general anaesthetic using ultrasound guidance. Brachytherapy is not advocated for all patients. In general, it may be considered for patients with low and intermediate grade disease, a small to moderate sized prostate gland, good urinary flow rates and a low PSA.
Further resources
- Cancer Research UK: Prostate cancer statistics.https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/prostate-cancer
- Prostate Cancer UK Charity. https://prostatecanceruk.org/prostate-information
- Macmillan Cancer Support. https://www.macmillan.org.uk/cancer-information-and-support/prostate-cancer
- NICE Clinical Knowledge Summary. Prostate Cancer. https://cks.nice.org.uk/prostate-cancer